Knee osteoarthritis is the most common type of osteoarthritis. More than 10 million Americans have knee osteoarthritis. It is also the most common cause of disability in the United States. Early diagnosis and treatment help manage knee osteoarthritis symptoms. An overview of knee osteoarthritis will help you understand symptoms, diagnosis, and treatment options.
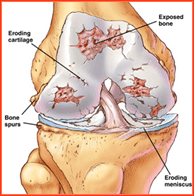
Deterioration of articular cartilage is the main problem associated with knee osteoarthritis. The condition can be caused by:
1. previous knee injury
2. repetitive strain on the knee
3. fractures, ligament tear, and meniscal injury which can affect alignment and promote wear and tear
4. genetics which make some people more likely to develop knee osteoarthritis
5. obesity
6. problems with subchondral bone (the bone layer underneath cartilage)
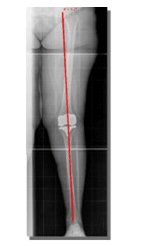
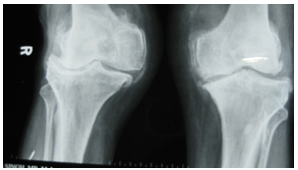
Medical history, physical examination, and x-rays are used to diagnose knee osteoarthritis. X-rays are very helpful, allowing the doctor to see evidence of joint space narrowing and rule out other causes of knee pain. If more detailed imaging is needed, an MRI may be ordered. Arthroscopic knee surgery is another way to view the condition of the knee.
Knee osteoarthritis typically develops gradually over a period of years. The primary symptoms associated with knee osteoarthritis include:
1. pain (mild, moderate, or severe)
stiffness
2. limited range of motion in the knee
3. localized swelling
Knee osteoarthritis pain is usually worse following activity, especially overuse of the affected knee. Stiffness can worsen after sitting for prolonged periods of time. As knee osteoarthritis progresses, symptoms generally become more severe. Pain can become continuous rather than only when weight-bearing.
The diagnosis of OA can usually be made on the basis of the initial history and examination. X-rays can help in the diagnosis and may be the only special test required in the majority of cases. X-rays can also help doctors rule out other problems, since knee pain from OA may be confused with other common causes of knee pain, such as a torn meniscus or kneecap problems. In some cases of early OA, X-rays may not show the expected changes.
Magnetic resonance imaging (MRI) may be ordered to look at the knee more closely. An MRI scan is a special radiological test that uses magnetic waves to create pictures that look like slices of the knee. The MRI scan shows the bones, ligaments, articular cartilage, and menisci. The MRI scan is painless and requires no needles or dye.
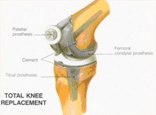
A total knee replacement is a surgical procedure whereby the diseased knee joint is replaced with artificial material. The knee is a hinge joint which provides motion at the point where the thigh meets the lower leg. The thigh bone (or femur) abuts the large bone of the lower leg (tibia) at the knee joint. During a total knee replacement, the end of the femur bone is removed and replaced with a metal shell. The end of the lower leg bone (tibia) is also removed and replaced with a channeled plastic piece with a metal stem or a separate plastic and metal shell (depending upon type of implant used).
The posterior cruciate ligament is a tissue that normally stabilizes each side of the knee joint so that the lower leg cannot slide backward in relation to the thigh bone. In total knee replacement surgery, this ligament is either retained, sacrificed, or substituted by a polyethylene post. Each of these various designs of total knee replacement has its benefits and risks. Total knee replacement surgery is considered for patients whose knee joints have been damaged by either progressive arthritis, trauma, or other rare destructive diseases of the joint. The most common reason for knee replacement in India is severe osteoarthritis followed closely by Rheumatoid arthritis of the knees. Regardless of the cause of the damage to the joint, the resulting progressive pain and stiffness, and decreasing daily function often leads the patient to consider total knee replacement. Decisions regarding whether to undergo knee replacement surgery are not easy. Patients should understand the risks as well as the benefits before making these decisions.A detailed discussion with your surgeon will help arrive at a decision especially when there are so many implant choices now available!
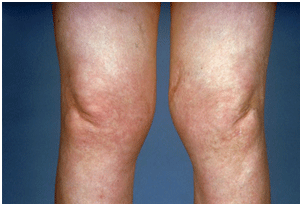
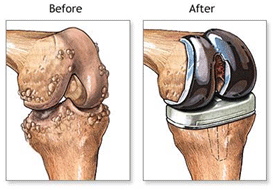
Your knee joint is made up of the ends of the thigh bone (femur) and shin bone (tibia), which normally glide over each other smoothly because they are covered by smooth articular cartilage. The joint is held in place by ligaments and covered at the front by the patella (kneecap). If the cartilage is damaged by injury or worn away by arthritis for example, the ends of the bones can rub together, causing pain and restricting movement. If this happens, your knee joint can be replaced with a prosthetic one.
There are several different types of knee replacement. Some need special bone cement to keep them in place. Other types of artificial knee parts are coated with a chemical which encourages bone to grow into it to hold the components in place
A growing number of surgeons are using camera-computer systems to help them apply their skills to the utmost advantage for patients undergoing joint replacement. The goal is to assist surgeons to operate with smaller incisions and greater precision.
Computer-assisted surgery helps surgeons align the patient's bones and joint implants with a degree of accuracy not possible with the naked eye. For the first time doctors have detailed information allowing them to balance the ligaments and it is given to them before they make the necessary cuts. The computers also help doctors who use smaller incisions instead of the traditional larger openings. Small-incision surgery, most often referred to as minimally invasive surgery, offers the potential for faster recovery, less bleeding and less pain for patients.
Think of it this way. Perhaps you've seen the on-board computers in newer cars that provide driving directions using satellite navigation systems. On-board computers collect data points from satellites and use precise coordinates to give drivers directions from point A to point B. It provides a degree of precision, speed and accuracy not attainable with a map and compass. Similarly, computers used during orthopaedic surgeries offer visual mapping to help doctors make crucial decisions before and throughout the operation. The systems are currently used for knee replacement surgeries. However, programs are being developed for hip replacement and other common orthopaedic procedures. The objective is to combine the precision and accuracy of computer technology with the surgeon's skill to perform surgery.
An advantage is that the doctor has greater "vision" when it counts during surgery. This supports decision-making and enhances the surgeon's flexibility. Here's how it works. Computer-assisted surgery uses:
1. The computer system
2. Cameras
3. Software
4. Specialized surgical instruments
5. Physician training
Doctors typically undergo special training to use computer assisted technology. DePuy Orthopaedics, Inc. refers to this category of surgery as iOrthopaedics, or Intelligent Orthopaedics, and requires users of their computer navigated system, the CiTM System, to go through one of their training centers before use.
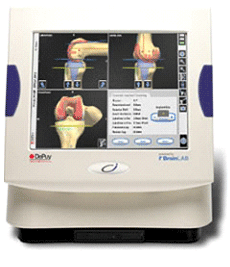
The Ci System captures the patient's unique anatomy and translates it to a computer screen, providing an unobstructed view of the patient's knee joint. The software and instrumentation of the Ci System are designed to work together. (Some systems use traditional surgical tools that must be adapted for use with computers). Imaging technology allows the surgeon to see a computer generated picture representation of a patient's bones allowing them the potential to operate with smaller openings and with more accuracy to reduce malalignment. The Ci System's lightweight, wireless computer system is used with a small camera array. A digital model is produced that serves as a map for each operation. The cameras take data via infrared signals from reflectors placed on the patient's body and on specially designed surgical instruments. The computer uses the data to track the exact position of the patient and the instruments on a monitor. The combination of computer visualization and special surgical instruments allows doctors to align the implant with greater precision than when doing the procedure with the naked eye.
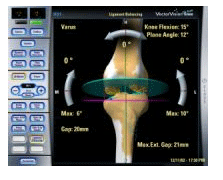
Whether the procedure includes or does not include computer support, joint replacement surgery is not for everyone. Recovery takes time and hard work. The life of a new joint depends on weight, activity level, age and other factors. Each patient responds differently. The most common adverse events include loosening, wear of components, osteolysis, infection, fracture, dislocation and tissue reaction. Advocates of the technology say they expect the use of computer-aided surgery to spread rapidly in the next decade because of the following potential benefits:
1. Support for the doctor in pre-operative planning.
2. Intra-operative flexibility to adapt the plan based on the data shown during the surgery.
3. Improved surgical accuracy and consistency.
The future of computer-assisted surgery is exciting and promising. Total joint replacement is a proven procedure that has been successful for decades in helping people live with less pain and greater mobility. Some surgeons will adapt the technology right away; others will await further results while adhering to the traditional hands-on approach they've used for years. As with any medical treatment, individual results may vary. Only an orthopaedic surgeon can determine whether an orthopaedic implant is an appropriate course of treatment. There are potential risks, and recovery takes time. The performance of the new joint depends on weight, activity level, age and other factors.